Diagnostics of Eye Disorders
Autorefractor keratometer
The autorefractor keratometer is a computerised system used to examine the refractive ability of the optical system of the eye to detect refractive disorders of the eye (myopia or near-sightedness, hyperopia or far-sightedness and astigmatism). Using the data obtained, an ophthalmologist or optometrist can select the optimum means of correction of refractive pathology in the form of eyeglasses or contact lenses more precisely.
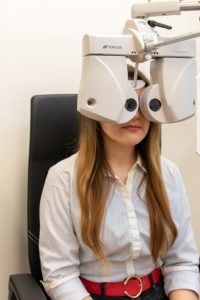
Digital foropter
The digital foropter is a device used to examine visual functions, determine visual acuity, select eyeglasses according to the dioptre strength, detect functions of binocular vision, examine double vision (diplopia), check colour vision and test contrast sensitivity. Use of a digital foropter allows conducting all these tests considerably faster.
Tonometer
Tonometers of the latest generation are built into autorefractor keratometers and are combined with a pachymeter, a device used to measure the thickness of the eye cornea. The thickness of the eye cornea must always be taken into account when assessing intra-ocular pressure (IOP) values. Use of several devices combined into a single device provides immediate automatic information on the real intra-ocular pressure (pressure adjusted according to the measurements of corneal parameters) of the patient.
Contactless tonometry is used as a screening method. Where a patient has elevated intra-ocular pressure according to contactless tonometry measurements, the pressure measurements should be done using contact tonometry techniques, e.g. iCare tonometry which is available at the Medicīnas centrs ARS Ophthalmology Facility.
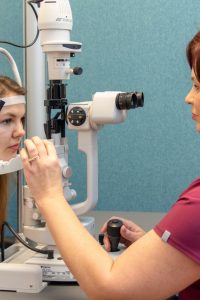
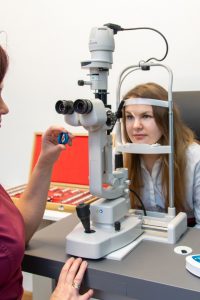
Biomicroscopy
A method used to examine and evaluate the front and back sections of the eye which are inspected using a special lens placed before the eye. Eye drops which dilate the pupils are used before the exam for a complete examination of the retina. This results in blurred vision for 2-4 hours, especially at close distances, and the eyes are more sensitive to light during this period, therefore a visit to the doctor should be planned so as to ensure that the exam does not affect the tasks to be performed during the rest of the day, including driving a car. Sometimes fluorescein in the form of orange droplets has to be used to diagnose corneal damage; the white part of the eye (sclera) may turn yellowish for a short time as a result.
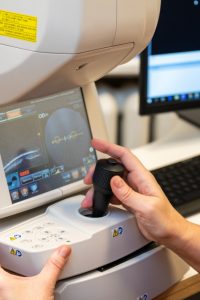
Computer perimetrytest (visual field test)
A method used to determine the visual fields (central and peripheral) of the eye. This exam plays an important role in diagnosticating glaucoma and assessing its progression as well as in evaluating the efficacy of treatment. It helps diagnose neurological pathologies and is also used in case of retinal disorders. The visual field test is also performed on drivers of motorised vehicles.
Optical coherence tomography (OCT)
A method of structural examination of the optic nerve, retina and cornea of the eye. It enables taking photos of the back of the eye and analysing these structures of the eye in cross-section. It also helps analyse the features of the surface of the retina, the structure of the retina, the thickness of the retinal nerve fibre layer. The exam is painless, without contact with the surface of the eye, and is safe for the patient’s health. No pupil-dilating eye drops have to be used during this exam.
This exam should be performed in case of suspicion of disorders of the optic nerve and retina of the eye. OCT is used in diagnosticating glaucoma and retinal disorders (age-related macular degeneration (AMD), diabetic macular oedema etc.), monitoring disease progression and in evaluating therapy.
Dioptrimetry
This exam helps determine the dioptre settings of eyeglass lenses. Analysis of monofocal (spherical and cylindrical), bifocal and progressive eyeglass lenses is possible. Using the data obtained, an ophthalmologist or optometrist assesses whether the eyeglasses used currently are appropriate and prescribes new ones if necessary.